In the last twelve years, scientists have published multiple studies that prove the honest placebo or open label concept, in which patients are informed in advance that the pill they are taking does not contain therapeutically active ingredients.
That was the case for Betty Durkin, who lived for days in excruciating pain after slipping at home. That fateful day, details for an interview with The National Geographic, her upper cervical spine was injured, splinters were stuck in her face, and her wrists and knees were severely bruised.
After receiving opioids 24 hours a day, something that really worried her because she had seen how a close friend had become addicted to these painkillers after two hospital stays, the opportunity came to participate in this unusual clinical trial: they would test if their pain improved after receiving a placebo pill with soybean oil instead of a medicinal ingredient.
In Durkin’s case, not only was she explicitly told what the treatment was like, but the bottle directly read “open-label placebo.”
Based on everything scientists believed for years – that concealment was the key to effective placebos – these pills were not going to reduce Durkin’s pain, fatigue, migraines or other symptoms. Yet the result it was quite different.
For three days, as part of the trial, Durkin sniffed cardamom spice before downing her opioid capsule. The goal was to train the brain to associate the experience of taking the placebo with pain relief from the opioids. On the third day, she was given the aroma and the capsule, but without opiates. She was told that she could ask for painkillers when she needed them, but she never did.
“I didn’t expect it to work. I knew it was a fake pill, not something active,” says Durkin. “But somehow my brain didn’t know the difference.”
According to the collection of National Geographic, a systematic review published last year in Scientific Reports evaluated 13 studies with almost 800 participants and concluded that open placebos have significant positive effects.
The reviewers cautioned, however, that in the early stages of research in any field, positive studies are more likely to be published than those that do not support the technique. Still, the unexpected effect has many medical experts intrigued.
“It’s a paradoxical intervention,” says Ted Kaptchuk, director of the therapeutic meeting and placebo studies program at Beth Israel Deaconess Medical Center in Boston and pioneer in this research. At first glance, it doesn’t make sense, he says, but that may be because scientists don’t fully understand how placebos work.
Since the 19th century, the word placebo has been used to refer to a false treatment, that is, one that does not contain any active physical substance. You may have heard of placebos as “sugar pills”.
The use of placebos in clinical trials really took off in the 1960s, after Congress passed an amendment authorizing the US Food and Drug Administration to require drug companies to show that new drugs not only they were safe, but also effective.
Clinical trials comparing a drug to a harmless placebo have become the accepted way to do it, the scientists noted in the New England Journal of Medicine on the 50th anniversary of the amendment.
In traditional clinical trials, participants are never told whether they are receiving the drug or the placebo. The scientists evaluating the trial data are also not informed, so the results are assumed to be more directly comparable and less likely to introduce bias.
Kaptchuk and colleagues enrolled 80 people with irritable bowel syndrome in a randomized clinical trial; half took two placebo capsules twice a day, and the rest received no treatment.
The researchers were careful to explain to the placebo group that the capsules did not contain any medication. They were also told that clinical trials have shown that placebos can induce self-healing processes.
After three weeks, the researchers assessed the severity of the symptoms. Kaptchuk’s team published a report showing that the placebo group improved significantly, a finding that opened the door for further research.
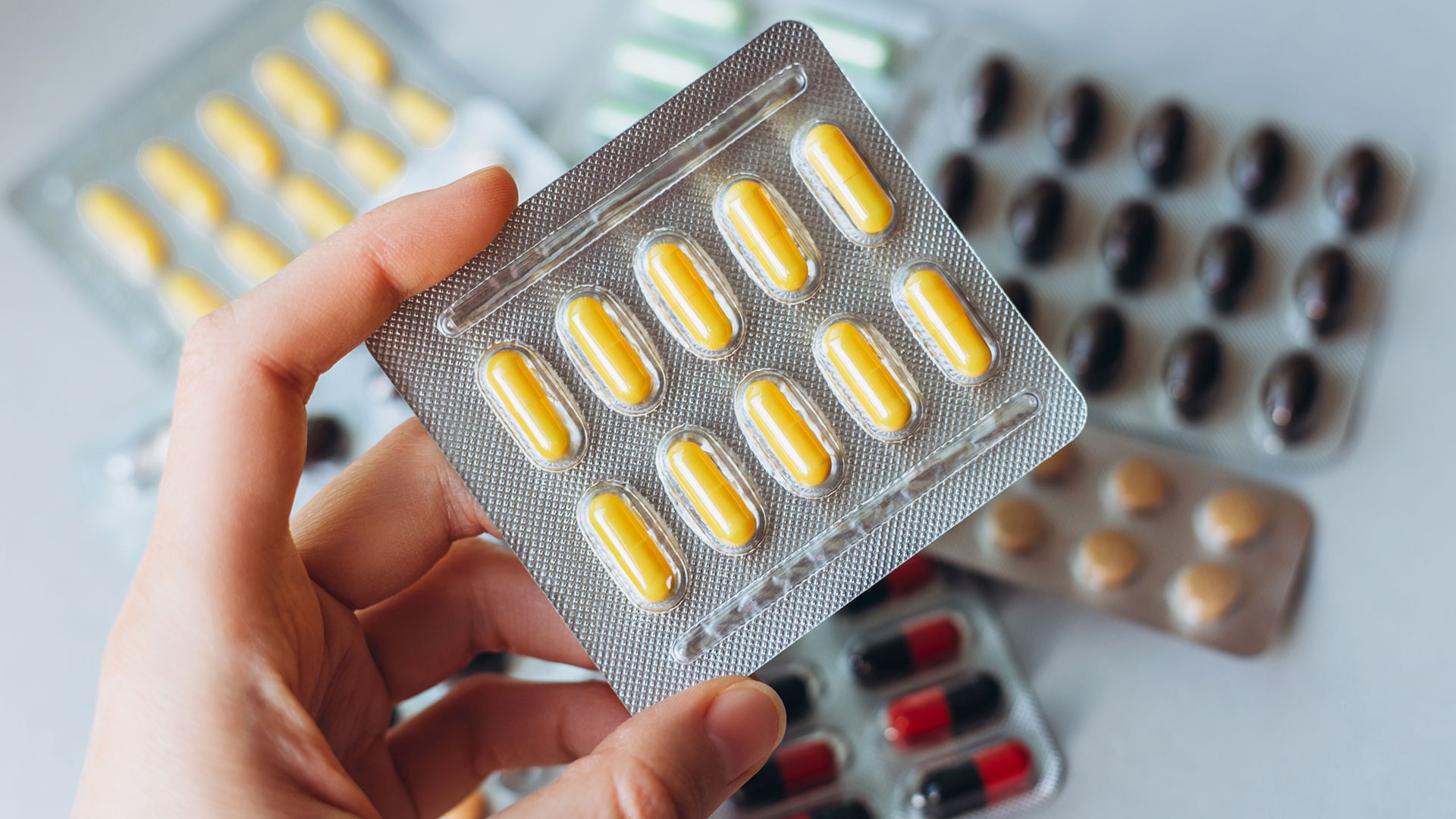
“I didn’t expect it to work. I knew it was a fake pill, but my brain didn’t know the difference,” said Betty Durkin, who participated in the clinical trial at the Spaulding Hospital in Boston.
Informing patients about the possible benefits of taking a placebo is crucial in open-label clinical research, says Leon Morales-Queezada, a physician at Spaulding Hospital in Boston who was the principal investigator of the study in which Durkin participated.
“We told our patients from the beginning: We’re going to give you a placebo, but there’s a chance it could help you control your pain and decrease your opioid use,” he says.
At first, people were surprised — and often skeptical — Morales-Quezada says. “They couldn’t believe what we were proposing. But at the same time they were curious”.
Clearly labeled placebos may work somewhat differently than their more traditional cousins. Experts are better understanding that, especially for pain patients, the brain can exacerbate pain and amplify bodily sensations that it should otherwise ignore.
In some people, the message of being instructed to swallow a pill with no physiological effects might somewhat disrupt the brain’s pain signal more than being told the placebo might be a drug, Kaptchuk wrote in the British Medical Journal in 2018.
“The placebo has nothing to do with the pill. It is the ritual of the pill,” says Kaptchuk. “It’s not about believing that it’s going to get better,” Kaptchuk conjectures. “In my opinion, it is about the body knowing something that it is not aware of.”

:quality(85)//cloudfront-us-east-1.images.arcpublishing.com/infobae/WZTEOCQQM5APNJEYJZ5R3QVB7A.jpg)