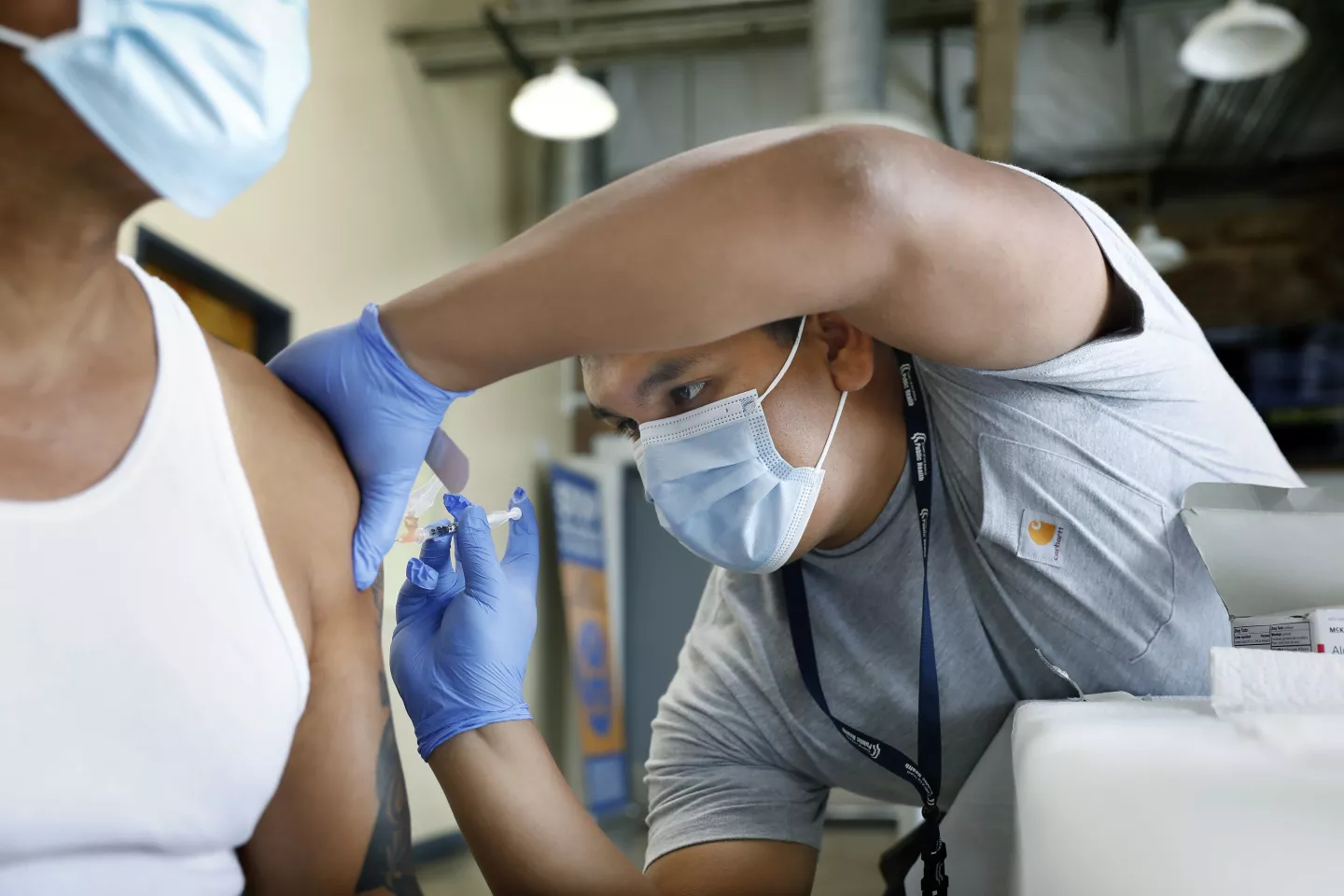
The formal end of the pandemic on May 11 marks neither victory nor peace: it is a cessation of hostilities with a dangerous virus that is still very much with us.
To maintain such an uneasy truce, Americans will have to remain sufficiently protected to prevent humanity’s viral enemy from staging a breakdown of our shaky arrangement.
Providing that assurance, in turn, assumes that scientists and public health officials agree on what it means to be “sufficiently protected” and that they can tell whether people are hitting that mark.
On both counts, the nation’s willingness to monitor this armistice falls short.
There are some reassuring trends. COVID-19 hospitalizations have plummeted, and weekly COVID-19 deaths have fallen 90% from their most recent peak just over a year ago.
But that’s just “a snapshot in time,” said Dr. Cody Meissner, a Dartmouth University pediatric infectious disease physician who serves on the FDA’s vaccine advisory panel. The pandemic virus’ ability to spring surprises makes scientists want to understand COVID-19 immunity well enough to anticipate its next move.
Scientists have a measure of immunity backed by decades of research: counting antibodies. It is easy and inexpensive to do so with readily available laboratory tests.
Gathering immune proteins that form following vaccination or infection is one way to assess how quickly a person can be expected to block or clear an infection. The more antibodies, the more complete your protection.
To gain information about the immunity of the nation as a whole, scientists measure antibodies to coronavirus in large groups of people, such as patients who had blood drawn for routine laboratory tests or volunteers who donated to blood banks. These seroprevalence surveys have shown that by June 2022, 94% of U.S. adults, and about the same number of children, had been vaccinated, infected, or both.
For a time, officials had hoped that high antibody levels would drive the virus out of circulation entirely. Once enough Americans were vaccinated, the reasoning went, the antibodies would block so many infections that the coronavirus would simply die out for lack of new victims to infect.
But as the pandemic unfolded, hopes of achieving this state of “herd immunity” faded.
All virus-specific antibodies “decay” over time, leaving behind a template to produce more when needed. But that renewal process takes time, and the Delta and Omicron variants proved apt to establish infections before the body’s defenses are in place.
Over time, it became clear that antibodies alone did not tell the whole story of Americans’ immunity. People who had been vaccinated or previously infected contracted COVID-19. But they did not become seriously ill or die at nearly the same rate as people who had no immune protection. Some other process was clearly at work.
That invisible mechanism was what scientists call cell-mediated immunity, and its foot soldiers are T cells.
Dr. Dan H. Barouch, a Harvard immunologist, calls T cells “the unsung heroes” of the immune system. They do the close-up job of hunting down and killing cells that have been invaded and hijacked by the coronavirus.
Cell-mediated immunity is widely credited with staving off the worst ravages of COVID-19. Even for those whose weakened immune systems generated an anemic antibody response to vaccination, cell-mediated immunity can be strongly activated and protect against death.
As the new mutations helped the coronavirus evade antibodies, T-cell responses appeared to remain strong against the new variants, including the many Omicron strains.
There is also encouraging evidence that this cell-mediated immunity is durable. Scientists have confirmed strong T-cell responses one year after SARS-CoV-2 infection and at least six months after vaccination. In addition, patients infected with the SARS-CoV coronavirus, a close relative of the pandemic virus responsible for the 2003 outbreak of severe acute respiratory syndrome, have shown signs of T-cell immunity 17 years later.
All of this has prompted University of Pennsylvania vaccine expert Dr. Paul Offit to question the value of repeated booster vaccines as a means of maintaining Americans’ protection against COVID-19.
Evidence has mounted that immunity for most Americans now relies more on T cells than on boosting antibody levels, Offit said. As a result, the U.S. government’s strategy of repeated booster vaccines is probably unnecessary for all but patients with weakened immune systems, he added.
Offit acknowledged that each injection boosts antibody levels. But it’s not clear that those additional antibodies reduce the likelihood of serious illness or death, which should now be the definition of “protected,” he said.
Meissner goes further.
“This virus is like the wind: you can’t stop the wind,” he said. “It’s going to continue to mutate and become more infectious. But as long as we can protect against serious illness at this stage of the pandemic, I can live with that.”
At a recent meeting convened by the FDA to consider vaccine strategies going forward, Offit, Meissner and others challenged the agency to make clear what the shots are intended to achieve and what metrics it will use to judge them.
“We need to define what we want from this vaccine,” Offit said at the meeting. If it is to protect against serious disease and death, “T cells are important.”
Unfortunately, the state of a person’s cellular immunity is more difficult to capture and quantify. There are tests that measure these immune cells, but they are not inexpensive or simple to perform.
The inhabitants of the cellular immune system are a diverse group whose functions change with time and circumstance. Key details about how this complex system responds to coronavirus still elude scientists, Meissner said.
There are tests that capture cell-mediated immunity, but they are very expensive to run. Most require a large volume of a person’s blood, special chemical reagents and complex manipulation to produce results. Many require highly skilled laboratory workers or extensive computational resources to generate useful data.
As a result, they are used sparingly in the treatment of patients. And they are never used to assess broad populations.
If a laboratory test could measure cellular immunity as easily as antibodies, “that would spread like wildfire, because everyone is looking for one,” Meissner said.
Such a test could not only assess whether a person needs a booster shot; if widely used, it could spur a return to public health measures such as social distancing and wearing masks. If T-cell protections have declined in populations, it might even alert vaccine manufacturers that they need to update the composition of vaccines to better match the circulating strain.
One such test may be a start.
In August, the European Medicines Agency gave its approval to a commercial assay that offers a simple way for scientists and public health officials to measure T-cell immunity.
The announced use of the test is to give immunocompromised patients a readout on whether they are at high risk of becoming seriously ill or dying if they contract the coronavirus. But public health officials in Spain used it to assess the immunity of Madrid residents after most received the vaccine and several waves of COVID-19 spread through the city.
For 40 consecutive days, phlebotomists collected 100 blood samples per day. Each night, the samples were processed by a single lab technician working with a PCR machine, a standard fixture in virtually any commercial testing laboratory. The results provide a yes/no answer to the question of whether there is a cellular immune response to the SARS-CoV-2 virus.
“Even my 12-year-old son can take the test,” said Jordi Ochando, an immunologist at the Icahn School of Medicine at Mount Sinai in New York, who oversaw the Madrid survey. Results can be available a day after the blood draw and uploaded instantly for analysis, sharing and storage, he added.
Ochando got his answer quickly: at an average of 10 months after vaccination, 90.2% of the population tested still showed a cellular immune response to the pandemic virus.
But it is easy and inexpensive to use. In Europe, the cost per person is “on par with a standard PCR test” for COVID-19, said Hyris founder and CEO Stefano Lo Priore.
“It’s a way, the only scalable way we have now, to quantify cellular immunity,” said Ernesto Guccione, a Mount Sinai immunology researcher who helped design the test and has a patent pending.
Such a test could make it affordable to measure cell-mediated immunity in residents of a boarding school, nursing home or city, Lo Priore said. The results could help officials decide whether to abandon or reinstate public health measures, such as indoor facemask mandates, or guide the timing of booster vaccinations.
Eventually, Guccione said, the test could be used in conjunction with other trials to reveal more about how T cells protect and for how long. It must pass FDA approval before it can be marketed in the United States, a process the company is currently preparing for.
Guccione and Ochando now have their sights set on measuring T-cell immunity in New York City, which has repeatedly been the epicenter of the pandemic in the United States.
Los Angeles could be next, Ochando said.